Not Feeling Baby Move as Much in 8th Month
- Research article
- Open up Access
- Published:
Fetal movement in tardily pregnancy – a content analysis of women'southward experiences of how their unborn baby moved less or differently
BMC Pregnancy and Childbirth book xvi, Article number:127 (2016) Cite this article
Abstract
Groundwork
Pregnant women sometimes worry nearly their unborn baby's health, often due to decreased fetal movements. The aim of this written report was to examine how women, who consulted health care due to decreased fetal movements, depict how the infant had moved less or differently.
Methods
Women were recruited from all seven commitment wards in Stockholm, Sweden, during 1/one – 31/12 2014. The women completed a questionnaire after it was verified that the pregnancy was viable. A modified content analysis was used to analyse 876 questionnaires with the women's responses to, "Try to describe how your baby has moved less or had changes in move".
Results
4 categories and six subcategories were identified: "Frequency" (decreased frequency, absenteeism of kicks and move), "Intensity" (weaker fetal movements, indistinct fetal movements), "Character" (changed pattern of movements, slower movements) and "Duration". In addition to the responses categorised in accord with the question, the women besides mentioned how they had tried to stimulate the fetus to move and that they had difficulty in distinguishing fetal movements from contractions. Further, they described worry due to incidents related to inverse pattern of fetal movements.
Conclusion
Women reported changes in fetal movement concerning frequency, intensity, character and elapsing. The challenge from a clinical perspective is to inform pregnant women about fetal movements with the goal of minimizing unnecessary consultations whilst at the aforementioned time diminishing the length of pre-infirmary delay if the fetus is at run a risk of fetal compromise.
Trial registration
Not applicable.
Background
It is widely acknowledged that a pattern of regular movements is associated with fetal wellbeing [1]. Fetal movements tin can be defined as any discrete kick, flutter, swish or roll and are usually commencement perceived by the mother between 18 and 20 weeks of gestation [two]. The frequency of fetal movements reaches a plateau in gestational week 32 and stays at that level until nativity [3]. There is normally a variation in fetal movements with a broad range in the number of movements per hour [4]. The movements are normally absent during sleep and occur regularly throughout the day and night, normally lasting for 20–xl min. The slumber cycles rarely exceed ninety min in the normal and salubrious fetus [5]. Although the motion design of the individual fetus is unique, information technology is full general knowledge that decreased fetal movement is associated with adverse consequence, including stillbirth [half-dozen].
The graphic symbol of the movements changes when the pregnancy approaches delivery due to limited space in the uterus, merely the frequency and intensity will non usually decrease [iii]. In an interview study, forty term pregnant women with an upshot of a healthy baby described fetal movements during the past week. Almost all experienced fetal movements every bit "strong and powerful". Half of the women also described the movements as "large" (involving the whole body of the fetus). Some other common description was "slow" as in "tedious motion" and "stretching" or "turning". Some of the women stated that they were surprised how powerfully the fetus moved [7].
Several maternal factors may impair the ability to recognize fetal movement [eight]. Amniotic fluid volume [9], fetal position [10], having an anterior placenta [10, 11], smoking, being overweight [6] and nulliparity [6, 12] have been reported as such factors. Maternal factors which may enhance the ability to recognize movement are the opportunity to focus on the fetus and the absence of distracting noises [thirteen]. About 50 % of the meaning women in a study from Norway were sometimes worried about decreased fetal movements [14]. In a review article, information technology was constitute that between four and xv pct of pregnant women consult wellness care considering of a decrease in fetal movement in the third trimester [one]. The aim of the present study was to examine how women, who consulted health care due to decreased fetal movements after gestational calendar week 28, draw how the baby had moved less or differently.
Methods
Settings and participants
Women were recruited from all vii delivery wards in Stockholm, Sweden from 1st Jan to 31st Dec 2014, and were asked to complete a questionnaire. The inclusion criteria were women in gestational week 28 or more than who consulted wellness care due to concerns over decreased fetal movements, with the ability to sympathize Swedish or English and a normal cardiotocography (CTG). Non responders, inadequate answers, multiple pregnancies, undefined gestational week and unknown personal identity number were exclusion criteria (Fig. ane). In total, 3555 questionnaires were completed during the information collection period. Information drove was in progress while the first 1000 questionnaires were analysed. Xx-eight women completed ii questionnaires and three women filled in 3 questionnaires; they consulted health care more than than in one case during the data collection menses due to concerns over decreased fetal movements. Of the women, 672 (76.7 %) were anile 20–35 years, 582 (66.four %) had a higher or university level of education and 650 (74.ii %) of the women were born in Sweden (Table ane). All women gave birth to a live kid.
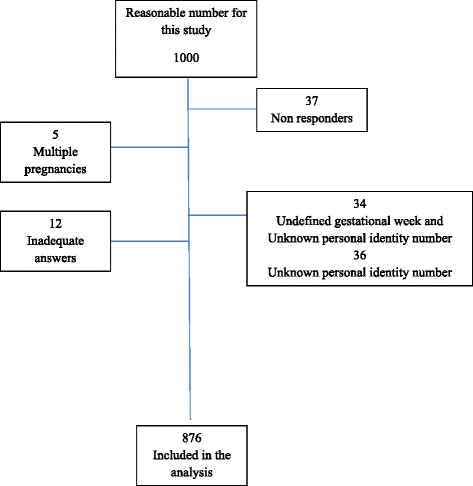
Menses chart
Data drove
The questionnaire used in the study was developed from a spider web survey, an interview study [7, 15] and clinical experience. The questionnaire was confront-to-face up validated with x women who consulted wellness care due to reduced fetal movements, not included in the study. The concluding version of the questionnaire included a total of 22 questions with multiple-choice or open up-ended response alternatives (Additional file one). This written report comprises the women's responses to the request: "Attempt to describe how your baby has moved less or had changes in movement". The women were asked to draw their experiences in the space provided but could also, if necessary, go along on the back of the questionnaire.
Analysis
The women'south descriptions (n = 876) of how their unborn infant had moved less or differently were analysed using a modified content analysis [sixteen]. The cloth consisted of concise descriptions of movements, which were used without editing. The analysis was performed in three steps. Firstly, all the answers were read and re-read iii times to gain a sense of content in the data. Codes were and then revealed in accordance with Malterud. Every quotation was read and sorted into codes. In the second phase of the assay the material was organized. Units, the quotations, with the same code were divided into defined principal categories and categories. When advisable the categories were divided into subcategories [17] The quotations could exist placed in more than than one category. Even so, each argument was only placed in one subcategory. During the whole process the findings were continually discussed in the research group in guild to reach agreement. To validate the results, a sample of 50 quotations was randomly selected and re-analysed from the beginning of the assay process. After consensus had been reached some of the quotations were transferred to other subcategories and three quotations were deemed irrelevant and removed. Those carrying out the analysis did not know the gestational calendar week.
Results
Iv main categories and half dozen subcategories were identified: "Frequency" (decreased frequency, absence of kicks and motion), "Intensity" (weaker fetal movements, indistinct fetal movements), "Character" (inverse blueprint of movements, slower movements) and "Elapsing". The number in each category and subcategory as well every bit an presentation of the figures for women seeking health care in gestational calendar week 28–32, gestational week 33–36 and during gestational week 37+, are shown in Tabular array two.
Frequency
The most ordinarily experienced deviation of fetal movements concerned frequency, which was described in 746 (85 %) of the questionnaires. This category was divided into two subcategories; "Decreased frequency" and "Absence of kicks and motion".
Decreased frequency of fetal motility
This subcategory comprises 609 (69 %) statements. These statements referred to movements becoming less frequent and indicating to the women a generally decreased liveliness in the fetus. The movements were described with words like, "a few", "seldom", "less frequent", "not as many" and "decreased action".
"Less frequent during the day"
"From beingness very active and kicking a lot to very few movements during some days"
Absence of kicks and movement
Among the answers about the frequency of fetal movements, 137 (16 %) statements were almost non feeling any motion at all.
"I oasis't felt any kicking for about 12 hours"
"Have not felt any motion during the whole day"
Intensity
A full of 343 (39 %) responses were perceptions that the movements had altered in intensity. Two subcategories were formed: "Weaker movements" and "Indistinct movements".
Weaker fetal movements
This subcategory comprised 277 (32 %) statements. Words frequently used were: "Weaker", "Softer", "Less sharp" and "With less power".
"From obvious, strong movements and nudging to feathery tickling a few times a day"
"… The movements of the baby felt weaker the few times I have felt my babe"
Indistinct fetal movements
Threescore-six (8 %) statements roughshod into this subcategory. Some women were uncertain equally to whether they felt anything at all simply thought they could imagine movements.
"…The but thing I felt was not-specific movements deep inside my tummy…"
"Have previously felt apparent kicks which can be both felt and seen distinctly. Since yesterday evening just small-scale occasionally twisting movements"
Character
This category comprised 252 (29 %) statements describing experiences of the fetal movements changing in character. The category revealed ii subcategories: "Inverse pattern of movements" and "Slower movements".
Inverse pattern of movements
This subcategory comprised 141 (xvi %) statements. The women described the fetal movements as having changed in pattern and decreased in action.
"Not the same pattern of movements as before and non active at the same time"
"The baby has not moved at the times that she had moved before, following the pattern that she had previously. This has been going on for about two days. When she has moved, the movements felt weaker the past 2 days compared to before."
Slower movements
This subcategory included 111 (13 %) statements. When talking virtually the movements women used words such as: "sluggish", "indolent", "slow and sweeping".
"Calmer more tired movements as if it were tired…"
"Ho-hum and smoother movements"
Duration
Thirty-eight (4 %) were included in this category. Women reported that the periods of motility had become shorter and had been reduced from several kicks in a row to occasional ones. Nevertheless, the frequency of how oft the infant had moved had non decreased.
"… the periods when it has moved have been shorter"
"No more lively periods."
Differences co-ordinate to gestational age
Women in gestational weeks 33–36 experienced changes more often than women at term regarding the category Frequency (92 % vs. 81 %), the subcategory Decreased frequency (75 % vs. 67 %), and the category Intensity (42 % vs. 35 %). Compared to women at term, those in gestational weeks 28–32 expressed changes to a lesser extent within the category Character and the subcategory Slower movements (5 % vs. 15 %) (Tabular array ii).
Iv per centum, 32/876, of the total number of women in this study only stated a modify in the grapheme of the movements, non included in any other category. The distribution regarding length of pregnancy was; gestational week 28–32, 1/190 (0.5 %), 33–36, i/263 (0.4 %) and gestational weeks 37+, 30/423 (7 %). In that location were no statistically significant differences in the other categories (Non in table).
In addition to the responses categorised in accordance with the question, the women also mentioned how they had tried to stimulate the fetus to move and that they had difficulty in distinguishing fetal movements from contractions. Farther, they described worry due to incidents related to inverse blueprint of fetal movements.
Stimulation due to less movement
We identified 146 (17 %) statements near trying to provoke movement by triggering the fetus. Well-nigh of the women reported that they did this when not having felt movements for a while. When they did not succeed they consulted health care. The methods used to trigger movements were to pull, nudge or button on the stomach, stimulate with lite or dissonance, have a shower or bathroom or to drink cold, sweet drinks. Others said that they had various positions they used to feel the baby more distinctly. Some women described not feeling movements without stimulating the baby.
"No pushes" dorsum when I am pulling on the tummy, no reaction when drinking a glass of lemonade. Otherwise he has been quite active and you have been able to see my tum moving"
"Even if I touch my tummy, swallow, drink, at that place is non much difference. He is moving considerably less"
Difficult to distinguish fetal movements from contractions
The women stated that the fetal movements ceased or changed in relation to contractions or that information technology was difficult to distinguish movements from contractions. Some women also described that the movements decreased in relation to contractions, hurting in the tummy or the back. Nosotros identified forty statements (five %) concerning difficulties in distinguishing fetal movements from contractions.
"Not felt any movements since the contractions became more intensive"
"Information technology has been more than difficult to perceive movements. Difficult to distinguish movements from contractions… previously the movements have been very distinct"
Worry due to incidents related to inverse pattern of fetal movements
We identified 25 (3 %) statements well-nigh external factors, such every bit the woman was sick and perceived less fetal movement. Six women stated that they consulted health intendance due to hurting in relation to inverse patterns of fetal movement. 2 statements referred to the adult female having taken a fall and wanting to exist reassured that the fetus had not been damaged. Other reasons related to increased worry were: post maturity, following an expelled mucus plug, an external cephalic version effort, rupture of the membranes and previous stillbirth in the same gestational calendar week.
"Used to move a lot during both day and nighttime. Have been sick with fever for iii days and then in that location have been movements iv–v times every twenty-four hours"
"Not every bit often every bit before just I even so experience him daily. We're extremely worried equally we lost our outset kid in gestational week 33 in utero so it may be imagination"
Discussion
We are not enlightened of any studies that accept categorized how women describe the changes they have perceived concerning fetal movements when they seek wellness care due to worry about their unborn babe.
Women who consulted health care due to decrease fetal movements described changes in frequency, intensity, character and duration of the movements. However, all women in this study were reassured after an exam of their unborn baby. In Norway, as many as 51 % of women reported that they were concerned well-nigh decreased fetal movements once or more in pregnancy [14]. In different populations, between four and 15 % consulted health intendance facilities because of decreased fetal movements in the third trimester [1]. There are several factors which may impair the power to recognize fetal movements [eight]. Even so, we take no data concerning amniotic fluid volume, fetal position, placenta position, smoking, overweight and nulliparity amidst the women participating in this written report. These factors may explain some of the women's perceptions of decreased fetal movements. Also, the plateau in gestational week 32 [3] may exist perceived every bit a decrease. In a study by Sheikh and colleagues (2014), 729 women counted and registered fetal movements for one hour iii times per day. 8 percent of the pregnant women in the tertiary trimester, who in the end gave birth to a healthy child, experienced reduced fetal movements. Further, the researchers institute that among women who consulted wellness care for reduced fetal movements but subsequently gave birth to a healthy kid, more of them were working than those who did not perceive reduced fetal movements [18]. We do not have information as to piece of work status among the women participating in our study.
Placental dysfunction is one main reason for decreased fetal movements in tardily pregnancy [19]. It is thus of import for the pregnant women to recognize the design of movement. A modify may be a sign of asphyxia due to the redistribution of the apportionment which gives priority to the brain over peripheral parts [twenty]. All fetuses in the present study were examined and no symptoms of asphyxia or placental dysfunction were identified at the time when the woman consulted health care. The women's worry about their unborn babe'south health due to decreased fetal movements in this study did not result in a diagnosis or actions to induce the commitment.
Our results indicate that some women at term seek health care due only to a change in the graphic symbol of the fetal movements. Although these women were asked to describe how their baby had moved less or differently, they did non mention a subtract in frequency in the fetal movements or a change in intensity. Dull, as in slow motion, stretching and turning, are descriptions of the character of fetal movements used by women in full term pregnancy, pregnancies that resulted in a healthy child [seven]. The women in our study who consulted health care simply due to a change in the character of the movements and not because of altered frequency and intensity might not have been enlightened of normal changes in the fetal motion patterns in tardily pregnancy. The changes they reported as unlike can be physiological due to limited space in the uterus at term [3]. There is no routine in Swedish antenatal health care for giving data about fetal movements only women are recommended to consult health intendance if they experience decreased fetal movements [21]. However, pregnant women ask for data virtually fetal movements in full general and for information about the number and type of fetal movements they tin look, equally well as how the movements are supposed to change over fourth dimension in pregnancy [22].
There were no stillbirths amongst the women in this study. Thus, we tin only speculate that information technology is possible that women who consult wellness care due to decreased or inverse patterns of fetal movement may be aware of the importance of detecting fetuses at risk as early equally possible. Detection of decreased fetal movements tin can improve the outcome and reduce filibuster in consulting health care [23, 24]. Further, the fetuses in this report who could be at take a chance were examined and adventure factors such as placental abruptions, growth retardation or malformations [25] may have been detected. The primary reason for consulting health care due to decreased fetal movements is worry about the health of the baby [xiv]. None of the women in our written report consulted health intendance without cause, but their worry was patently unfounded from a medical perspective in the brusque term.
Strengths and limitations
Women in this study had a normal CTG before they completed the questionnaire. However, aside from no stillbirths among the participating women, we have no data regarding the health status of the baby later nascence. This is a major limitation of the written report. At that place is also only sparse information nearly the women'due south' sociodemographic groundwork.
One strength of the study is the large number of participants. Some other force is that all commitment wards in Stockholm participated in the study. Nevertheless, all women came from the capital urban center in Sweden where women in generally are older and well educated compared with women outside the capital letter. Further, the number of those who declined to participate and their reasons for doing so are not known.
The wording of the request, "Try to describe how your baby has moved less or had changes in move" might take influenced the responders to apply the words "decreased" and "differently" in their descriptions of their experiences. The results may have yielded fifty-fifty more than if the initial request had been broader or more open, for example, "Endeavor to describe how your baby has moved". Yet, the context in which the women completed the questionnaire was one of already perceived decreased fetal movements.
Clinical implications
Increased cognition nearly the normal changes in the fetal movement patterns in late pregnancy tin be one way to lessen the number of visits to obstetric clinics from women over concerns that turn out to be unnecessary from a medical perspective. The challenge from a clinical perspective is to inform and suggest pregnant women nearly fetal movements with the goal of diminishing the length of pre-hospital filibuster if the fetus is at risk and at the aforementioned time reduce worry leading to unnecessary consultation. Reducing the pre-hospital delay when the intrauterine environs is a threat to the unborn infant's life volition provide a window of opportunity to salvage a greater number of children from death or compromised health. Further, fewer visits to obstetric clinics, over business that turns out to be unnecessary from a medical perspective, will have health economic benefits. Before giving definitive advice that can reduce unnecessary controls at the end of the pregnancy, distinct differences must be identified regarding how women who lost their child intrauterine or accept given birth to a hypoxic or anaemic kid, study the changes in character of movements as only symptoms when they seek care for decreased fetal movements. Time to come studies are needed.
Conclusions
Women reported changes in fetal motility concerning frequency, intensity, character and elapsing; they described decreased, absenteeism, weaker, slower and changed pattern of the movements.
References
-
Froen JF. A kick from within--fetal movement counting and the cancelled progress in antenatal intendance. J Perinat Med. 2004;32(1):xiii–24. doi:10.1515/JPM.2004.003.
-
Neldam Due south. Fetal movements as an indicator of fetal wellbeing. Lancet. 1980;1(8180):1222–4.
-
RCOG. Green-meridian guideline No.57: reduced fetal movements. London: Royal College of Obstetricians and Gynaecologists; 2011. http://www.rcog.org.united kingdom of great britain and northern ireland/womens-health/clinical-guidance/reduced-fetal-movementsgreen-tiptop-57. Accessed 17 May 2016.
-
Nowlan NC. Biomechanics of foetal movement. Eur Prison cell Mater. 2015;29:1–21. discussion.
-
Patrick J, Campbell Yard, Carmichael L, Natale R, Richardson B. Patterns of gross fetal body movements over 24-hour observation intervals during the terminal 10 weeks of pregnancy. Am J Obstet Gynecol. 1982;142(4):363–71.
-
Holm Tveit JV, Saastad E, Stray-Pedersen B, Bordahl PE, Froen JF. Maternal characteristics and pregnancy outcomes in women presenting with decreased fetal movements in late pregnancy. Acta Obstet Gynecol Scand. 2009;88(12):1345–51. doi:10.3109/00016340903348375.
-
Radestad I, Lindgren H. Women'south perceptions of fetal movements in full-term pregnancy. Sexual activity Reprod Healthc. 2012;3(three):113–6. doi:10.1016/j.srhc.2012.06.001.
-
Hijazi ZR, East CE. Factors affecting maternal perception of fetal motility. Obstet Gynecol Surv. 2009;64(7):489–97. doi:10.1097/OGX.0b013e3181a8237a. quiz 99.
-
Ahn MO, Phelan JP, Smith CV, Jacobs N, Rutherford SE. Antepartum fetal surveillance in the patient with decreased fetal move. Am J Obstet Gynecol. 1987;157(iv Pt ane):860–four.
-
Fisher ML. Reduced fetal movements: a research-based project. Br J Midwifery. 1999;seven:733–vii.
-
Fried AM. Distribution of the majority of the normal placenta. Review and classification of 800 cases by ultrasonography. Am J Obstet Gynecol. 1978;132(vi):675–lxxx.
-
Mohr Sasson A, Tsur A, Kalter A, Weissmann Brenner A, Gindes L, Weisz B. Reduced fetal movement: factors affecting maternal perception. J Matern Fetal Neonatal Med. 2015:one–4. doi:ten.3109/14767058.2015.1047335.
-
Johnson TR. Maternal perception and Doppler detection of fetal movement. Clin Perinatol. 1994;21(iv):765–77.
-
Saastad E, Ahlborg T, Froen JF. Low maternal awareness of fetal move is associated with small for gestational age infants. J Midwifery Womens Health. 2008;53(4):345–52. doi:10.1016/j.jmwh.2008.03.001.
-
Linde A, Pettersson K, Radestad I. Women's experiences of fetal movements before the confirmation of fetal death--contractions misinterpreted every bit fetal movement. Birth. 2015;42(2):189–94. doi:10.1111/birt.12151.
-
Malterud Chiliad. Shared understanding of the qualitative inquiry process. Guidelines for the medical researcher. Fam Pract. 1993;10(2):201–6.
-
Malterud K. Kvalitativa metoder i medicinsk forskning. 3rd ed. Lund: Studentlitteratur; 2014.
-
Sheikh M, Hantoushzadeh S, Shariat M. Maternal perception of decreased fetal movements from maternal and fetal perspectives, a cohort study. BMC Pregnancy Childbirth. 2014;14:286. doi:10.1186/1471-2393-14-286.
-
Scala C, Bhide A, Familiari A, Pagani Thousand, Khalil A, Papageorghiou A, et al. Number of episodes of reduced fetal movement at term: association with agin perinatal outcome. Am J Obstet Gynecol. 2015. doi:10.1016/j.ajog.2015.07.015.
-
Jensen A, Garnier Y, Berger R. Dynamics of fetal circulatory responses to hypoxia and asphyxia. Eur J Obstet Gynecol Reprod Biol. 1999;84(2):155–72.
-
SFOG. In: Lars-Åke M, editor. Mödrahälsovård, Sexuell och Reproduktiv Hälsa. Stockholm: Svensk Förening för Obstetrik och Gynekologi; 2008. p. 52.
-
McArdle A, Flenady V, Toohill J, Gamble J, Creedy D. How pregnant women learn about foetal movements: sources and preferences for information. Women Birth. 2015;28(ane):54–nine. doi:10.1016/j.wombi.2014.10.002.
-
Froen JF, Arnestad Grand, Frey K, Vege A, Saugstad OD, Devious-Pedersen B. Adventure factors for sudden intrauterine unexplained decease: epidemiologic characteristics of singleton cases in Oslo, Norway, 1986–1995. Am J Obstet Gynecol. 2001;184(4):694–702.
-
Grant A, Elbourne D, Valentin L, Alexander S. Routine formal fetal movement counting and risk of antepartum late death in unremarkably formed singletons. Lancet. 1989;2(8659):345–9.
-
Flenady V, Koopmans Fifty, Middleton P, Froen JF, Smith GC, Gibbons K, et al. Major risk factors for stillbirth in high-income countries: a systematic review and meta-analysis. Lancet. 2011;377(9774):1331–40. doi:10.1016/S0140-6736(10)62233-7.
Funding
The Lilliputian Child'south Foundation, Sophiahemmet Foundation, The Swedish National Infant Foundation and Capo'southward Research Foundation funded this study.
Availability of data and materials
The information volition not be fabricated available in order to protect the participant's identity.
Authors' contributions
AL, KP and IR participated in the pattern of the study. AL, SG and IR performed the qualitative analyses. SH and EN carried out the start and chief role of the analysis. KP contributed to the discussion of the analysis. AL, SG, KP and IR drafted all versions of the manuscript. AL, SG, KP, SH, EN and IR commented on the draft. All authors read and approved the last manuscript.
Competing interests
The authors declare that they accept no competing interests.
Consent for publication
Not applicative.
Ethics approval and consent to participate
The women gave consent to participate and permission to admission supporting data when receiving data about the study. The information will non be made available in order to protect the participant's identity. The study was approved by the Regional Ethical Review Board in Stockholm: DNR: 2013/1077-31/3.
Author data
Affiliations
Corresponding author
Additional file
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/past/4.0/), which permits unrestricted apply, distribution, and reproduction in any medium, provided y'all requite appropriate credit to the original author(south) and the source, provide a link to the Creative Commons license, and indicate if changes were fabricated. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this commodity, unless otherwise stated.
Reprints and Permissions
Most this commodity
Cite this article
Linde, A., Georgsson, S., Pettersson, Chiliad. et al. Fetal movement in late pregnancy – a content analysis of women's experiences of how their unborn baby moved less or differently. BMC Pregnancy Childbirth 16, 127 (2016). https://doi.org/10.1186/s12884-016-0922-z
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/10.1186/s12884-016-0922-z
Keywords
- Pregnancy
- Fetal movement
- Decreased fetal movements
- Content assay
Not Feeling Baby Move as Much in 8th Month
Source: https://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/s12884-016-0922-z
0 Response to "Not Feeling Baby Move as Much in 8th Month"
Post a Comment